Some excerpts from today’s briefing:
Oxfam is proposing two things that the G20 and other leaders can do simultaneously. The first is to develop a Global Public Health Plan and Emergency Response to tackle the disease head on – preventing and delaying its spread, saving lives now and into the future. The second is to create an economic rescue plan to pay for the huge increase in public health and to help ordinary people cope with the huge economic costs precipitated by this virus. This first media brief focuses on the Global Public Health Plan and Emergency Response.
According to the WHO, at least half the world’s 7.6 billion people cannot access the essential healthcare they need even in normal times. In developing countries, the disease burden is already far higher than in rich nations. Each day nearly 4,000 people die from tuberculosis; a further 1,500 are killed by malaria, most of them children.
These numbers are at risk of rising dramatically as the pandemic competes for stretched healthcare resources. Across low-income countries, the average health spending was only US$41 per person in 2017, compared with US$2,937 in high-income countries – more than 70 times greater. Weak, underfunded and unequal health systems in developing countries are already completely unable to cope.
A coordinated and massive investment in public health is desperately needed now if we are to stop the spread of this deadly virus and prevent millions of deaths.
Enlightened multilateralism, long sacrificed to narrow nationalism, must be put back at centre stage to build an emergency and long-term health response unseen in our history. The WHO should work with the G20 and other national governments to rapidly agree and fund a Global Public Health Plan and Emergency Response.
It would cost approximately $159bn to double the public health spending of all of world’s 85 poorest countries. These countries are home to 3.7 billion people. This is less than 8% of the latest US fiscal stimulus alone.
Rich countries can help developing countries in two key ways: by giving them aid and by reducing their existing costs and debts. A key start will be immediately to fully fund the $2bn UN Humanitarian Response Plan, and plan for a massive scaling up of global humanitarian efforts as the virus starts to impact the poorest countries.
This must include steps to provide clean water, public health education, and cash grants. Much of this funding needs to go directly to local NGOs, and special care must be taken to address the gendered impacts this crisis will have. Donors and multilateral institutions should also rapidly scale up other aid, building on initial moves from the World Bank, IMF and others, and especially provide support to developing country health budgets.
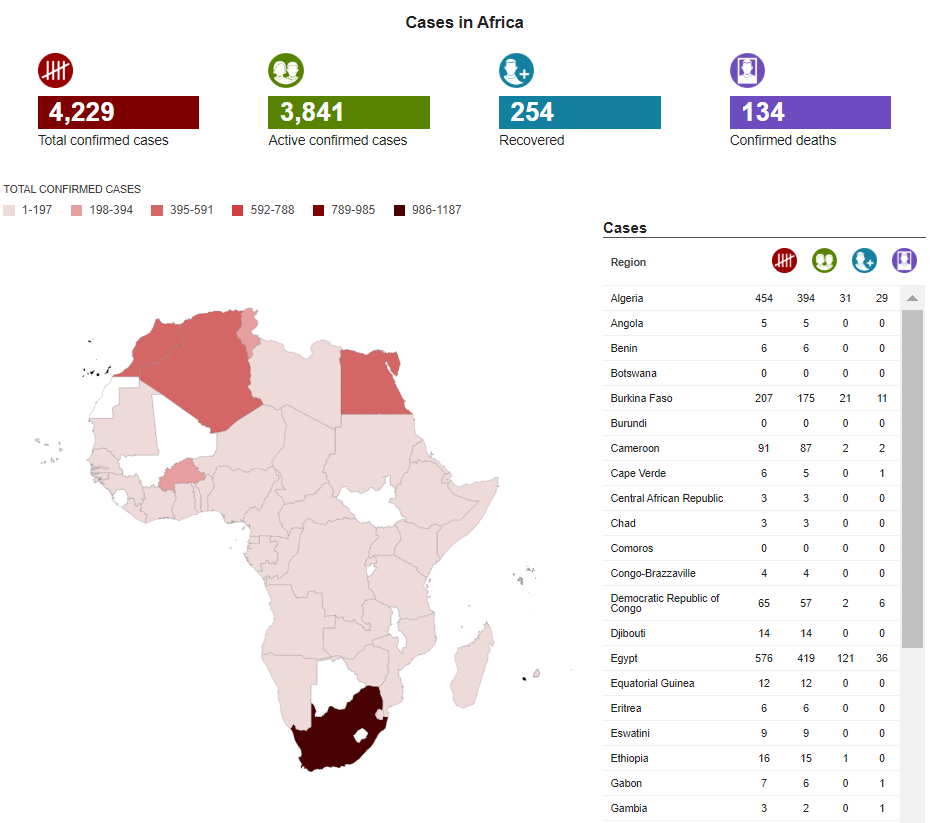
Second, the G20 and all bilateral and multilateral donors need to agree to an immediate moratorium on debt interest payments for poor country governments without conditions. This has already been called for by the World Bank and the IMF in an unprecedented move. In Africa alone, this act would free up an estimated $44bn this year to help finance their public health response.
So far, the outbreak has not spread extensively in developing countries, many of which have massive urban slum populations; but this is changing fast and is a huge public health challenge.
Immediate action is needed to shore up public health systems now and for the long-term, making them fair and accessible to all and saving millions of lives:
1. Prevention. Huge investments must be made in prevention: public health promotion and communication, community engagement and education, and in access to water and sanitation, especially handwashing, as well as free testing for all.
2. Ten million health workers. Ten million new paid and protected health workers should be recruited to help slow the spread of this virus and to be there to treat and care for those affected.
3. Free healthcare. Governments must remove all financial barriers to people accessing healthcare and deliver free testing and treatment to all who need it.
4. Private must work for public. Governments must requisition or find other means to utilize all private healthcare facilities to increase capacity to treat and care for infected patients and to meet ongoing essential health needs.
5. Vaccine and treatment for all. Global agreement must be reached that vaccines and treatments, when discovered, will be a global public good, available to all who need it for free and that rich countries will provide enough funding to make it available rapidly to the whole of humanity.
The full briefing is here.